Table of Contents
- What Is HPV Self-Sampling?
- Why HPV Self-Sampling Matters
- How HPV Self-Sampling Works
- Is HPV Self-Sampling Accurate?
- Who Should Consider HPV Self-Sampling?
- Types of HPV Self-Sampling Devices
- Benefits of HPV Self-Sampling
- What Happens After a Positive Result?
- Global Recommendations and Progress
- Limitations and Safety Points
- Frequently Asked Questions
- Conclusion
1. What Is HPV Self-Sampling ?
HPV self-sampling is a simple, private method that allows women to collect their own vaginal sample for human papillomavirus (HPV) testing without visiting a doctor for a pelvic exam.
Using a small brush or swab, a woman gently takes a sample herself. That sample is then sent to a certified laboratory for HPV DNA testing.
No speculum is needed. No clinic appointment is required. The process takes just a few minutes and can be done at home or in a healthcare setting, depending on your country’s guidelines.
HPV self-sampling is now recognized globally as one of the most effective ways to expand cervical cancer screening, especially for women who have never been tested.
2. Why HPV Self-Sampling Matters
Cervical cancer is almost entirely preventable, yet it remains a leading cause of cancer deaths among women worldwide.
In 2022, there were an estimated 662,301 new cases and 348,874 deaths from cervical cancer globally. The main driver is persistent infection with high-risk HPV types, the same infection that HPV self-sampling detects early.
The core problem is that millions of women never get screened. Common reasons include:
- Fear of pelvic examinations
- Cultural or religious concerns
- Embarrassment or past trauma
- Living far from clinics
- Lack of time or healthcare access
HPV self-sampling directly removes these barriers. It gives women full control over when, where, and how they get screened.
The World Health Organization has set a global target of 70% screening coverage by 2030. HPV self-sampling is considered a key tool for reaching that goal.
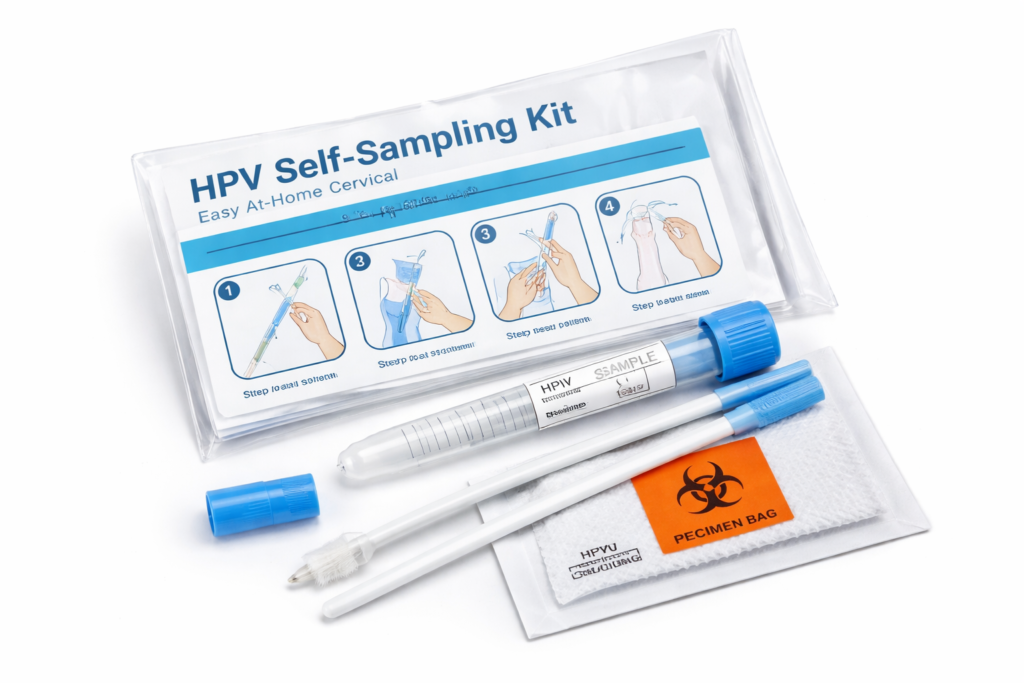
3. How HPV Self-Sampling Works
The process is clear and straightforward. Here is what to expect:
Step 1 - Receive your kit.
A self-sampling kit arrives by post or is collected from a clinic, pharmacy, or community health centre. It contains a sterile swab or brush, a collection tube, and instructions.
Step 2 - Collect the sample.
Insert the swab gently into the vagina and rotate for a few seconds to collect cells. The process is usually painless and takes under two minutes.
Step 3 - Package and send.
Place the swab in the provided tube and seal it. Mail it to the certified laboratory or drop it off as directed.
Step 4 - Receive your results.
Results are usually available within a few weeks.
- Negative result: No high-risk HPV detected. Continue routine screening as recommended.
- Positive result: High-risk HPV was found. Further evaluation by a clinician is required.
4. Is HPV Self-Sampling Accurate?
This is one of the most important questions, and the evidence is very reassuring.
Research consistently shows that HPV self-sampling performs comparably to clinician-collected samples when validated DNA testing methods are used.
A major 2025 meta-analysis reviewed 67 studies covering 18,615 women aged 15 to 80. The results showed:
- Sensitivity: 87.4% – correctly identifies HPV when it is present
- Specificity: 91.2% – correctly rules out HPV when it is absent
These figures confirm that HPV self-sampling is not inferior to samples collected by a doctor.
A large Asian systematic review covering 117,279 women also found high consistency between self-collected and clinician-collected samples. Agreement values exceeded 0.7 in most studies – considered statistically strong.
In the United States, the FDA has approved two specific tests, Onclarity HPV (Becton Dickinson) and cobas HPV (Roche), for use with self-collected vaginal samples in healthcare settings.
The NCI-led SHIP Trial is now underway to confirm that home-based collection performs equally well to clinic collection, with results expected to support future home approval.
5. Who Should Consider HPV Self-Sampling?
HPV self-sampling is suitable for a wide range of women. Most guidelines recommend it for women aged 30 to 65, although some programs start from age 25. Always follow your local screening recommendations.
It is especially helpful for:
- Women who have never been screened
- Women overdue for a cervical screening test
- Women in rural or remote areas with limited clinic access
- Women who feel anxious or uncomfortable with pelvic exams
- Women with past trauma or physical disabilities
- Women from communities with cultural barriers to clinical screening
HPV self-sampling is generally not recommended for:
- Pregnant women (in most study protocols)
- Women with current cervical cancer symptoms
- Women are currently under investigation for abnormal results
- Women who have had a hysterectomy (unless specified by a provider)
It is not a replacement for medical care – but it is a powerful first step for women who currently receive no screening at all.
6. Types of HPV Self-Sampling Devices
Several types of HPV self-sampling devices are available, and research shows they all perform well.
Device | How It Works |
Evalyn Brush | Small rotating brush that collects vaginal cells |
FLOQSwabs | Flocked nylon swab that absorbs and releases cells efficiently |
Multitest Kit | Combination collection and transport system |
M-Strip (menstrual) | Attaches to a sanitary pad; collects cells from menstrual blood |
A 2025 UK study tested five different workflows using DNA and mRNA HPV assays. Four of the five workflows showed sensitivity close to clinician-collected samples.
The M-Strip is a newer innovation being studied in India. One 2025 study reported 100% concordance with direct cervical smears. However, health authorities note that menstrual blood sampling still requires more research before it can be widely recommended.
For most women, a brush or swab-based kit remains the current standard.
7. Benefits of HPV Self-Sampling
HPV self-sampling offers clear advantages over traditional clinic-based cervical screening.
Benefit | Detail |
Privacy | Sample collected at home, in complete privacy |
Comfort | No speculum or pelvic exam required |
Convenience | No appointment needed; fits any schedule |
Accuracy | Proven comparable to clinician sampling in major trials |
Accessibility | Reaches rural, underserved, and marginalized communities |
Empowerment | Women take direct control of their own health |
Cost-Effective | Reduces clinic visits and healthcare system burden |
Studies consistently show that 62.8% of women prefer self-collection over clinician-collected sampling. Acceptance is high across different cultures, age groups, and healthcare settings.
8. What Happens After a Positive Result?
A positive HPV self-sampling result does not mean you have cancer. It means a high-risk HPV type was detected in your sample.
Here is what comes next:
- You will be asked to visit a clinic for a clinician-collected cervical sample.
- That sample is tested for abnormal cell changes (cytology).
- If abnormal cells are found, you may be referred for colposcopy – a closer examination of the cervix.
- If needed, treatment of pre-cancerous cells can prevent cancer from developing.
Most HPV infections clear up on their own and never lead to cancer. The goal of HPV self-sampling is to find and monitor high-risk infections before they cause harm.
In some programs, a “screen-and-treat” approach is used, allowing immediate treatment for screen-positive women without waiting for colposcopy. This is especially useful in low-resource settings.
9. Global Recommendations and Progress
HPV self-sampling is now part of official screening policies in multiple countries.
World Health Organization (WHO) The WHO recommends HPV DNA testing as the preferred method for cervical cancer screening. HPV self-sampling is endorsed as an effective tool to increase participation, particularly in underserved populations. 🔗 WHO HPV Screening Guidelines (Do Follow)
United Kingdom In March 2025, the UK National Screening Committee (UK NSC) recommended that cervical screening providers offer HPV self-sampling to women who never or rarely attend routine appointments. Evidence shows it is an effective and acceptable method to reduce health inequalities in screening coverage. 🔗 UK NSC Recommendation – June 2025 (Do Follow)
United States In May 2024, the FDA expanded approvals for two HPV tests — Onclarity HPV and cobas HPV — to include self-collected vaginal samples in healthcare settings such as clinics, urgent care centres, and pharmacies. 🔗 NCI – FDA HPV Self-Collection Approvals (Do Follow)
Australia and Netherlands Both countries have offered HPV self-sampling programs for years, with documented improvements in screening participation among hard-to-reach women.
Hong Kong In June 2024, Hong Kong launched a pilot scheme at 11 Maternal and Child Health Centres to test the feasibility and acceptability of HPV self-sampling in local communities. 🔗 CUHK – HPV Self-Sampling Program
India Researchers are actively studying community-based HPV self-sampling models. Studies highlight the urgent need for affordable, point-of-care HPV diagnostics and community education programs. 🔗 PMC Research – HPV Self-Sampling in Asia
10. Limitations and Safety Points
While HPV self-sampling is highly effective, it is important to understand what it can and cannot do.
It only tests for HPV. It does not detect other gynaecological conditions. Regular health check-ups with a doctor remain essential.
A positive result needs follow-up. HPV self-sampling is the first step, not the last. Any positive result must be followed up with a clinician.
Instructions matter. Samples collected incorrectly may be inadequate. Always read the kit instructions carefully. Many kits include picture guides or video links.
It does not replace vaccination. HPV vaccination and regular screening together provide the strongest protection against cervical cancer. Self-sampling is a screening tool, not a preventive treatment.
Cost and access gaps still exist. Although cheaper than clinic visits, kit costs and lab fees can still be a barrier. National programs are working to provide affordable or free access.
11. Conclusion
HPV self-sampling is one of the most important advances in women’s health in recent years.
It is accurate, accessible, acceptable, and proven to reach the women who need screening most. By removing fear, embarrassment, and logistical barriers, it gives every woman the chance at early detection – regardless of where she lives or what her circumstances are.
The evidence is clear. The global momentum is growing. Millions of women who were previously unreached are now getting the screening they need and deserve.
If you have been putting off cervical screening – for any reason – talk to your healthcare provider today about whether HPV self-sampling is available in your area.
Early detection saves lives. HPV self-sampling makes that detection possible for more women than ever before.
11. Frequently Asked Questions
Is HPV self-sampling painful?
No. Most women find it quick, easy, and comfortable. There is no speculum and no internal examination.
Can HPV self-sampling detect cancer?
It detects the presence of high-risk HPV types. Further clinical testing is needed to determine whether any cell changes have occurred.
How often should I do HPV self-sampling?
Most national guidelines recommend cervical screening every 5 years if results are negative. Follow your local guidelines.
Can I do HPV self-sampling at home?
In the UK, Australia, and Netherlands, home kits are available. In the US, self-collection is currently approved in healthcare settings, with home-based approval being studied through the SHIP Trial.
Is a negative result a guarantee I won't get cervical cancer?
No. A negative result is reassuring, but regular ongoing screening is still essential. HPV infections can develop at any time.
All Source References
- World Health Organization – HPV and Cervical Cancer Screening Guidelines https://www.who.int/publications/i/item/WHO-SRH-23.1
- National Institutes of Health / NCBI – Cervical Cancer Screening https://www.ncbi.nlm.nih.gov/books/NBK545378/
- CUHK – HPV Self-Sampling Pilot Programme, Hong Kong https://www.cuhk.edu.hk/sphpc/hpvselfsampling/en/self-samping.html
- National Cancer Institute – FDA HPV Self-Collection Approvals (2024) https://www.cancer.gov/news-events/cancer-currents-blog/2024/fda-hpv-test-self-collection-health-care-setting
- The Lancet Global Health – HPV Self-Sampling Systematic Review https://www.thelancet.com/journals/langlo/article/PIIS2214-109X(19)30067-1/fulltext
- PMC / NCBI – HPV Self-Sampling Research 2025 https://pmc.ncbi.nlm.nih.gov/articles/PMC11949917/
- BMJ Global Health – HPV Self-Sampling in Low- and Middle-Income Countries https://gh.bmj.com/content/6/5/e003743
- PubMed – HPV Self-Sampling Device Comparison Study https://pubmed.ncbi.nlm.nih.gov/39412108/
- UK National Screening Committee – HPV Self-Sampling Recommendation (June 2025) https://nationalscreening.blog.gov.uk/2025/06/24/uk-nsc-recommends-hpv-self-sampling-option-for-under-screened-women-in-cervical-screening-programme/
Public Health Disclaimer:
This article is for informational purposes only and does not replace professional medical advice. Always consult a qualified healthcare provider for guidance on cervical cancer screening.