Introduction:
Hospital acquired infections remain one of the most pressing concerns in modern healthcare. These infections, also known as healthcare-associated infections (HAIs), occur when patients develop illnesses during their stay in medical facilities. The alarming reality is that millions of patient’s worldwide contract these preventable infections each year, leading to prolonged hospital stays, increased medical costs, and tragic fatalities.
Every day, vulnerable patients enter hospitals seeking healing, yet many unknowingly face risks from these dangerous infections. Understanding what hospital acquired infections are, how they spread, and most importantly, how to prevent them can literally save lives.
What Are Hospital Acquired Infections?
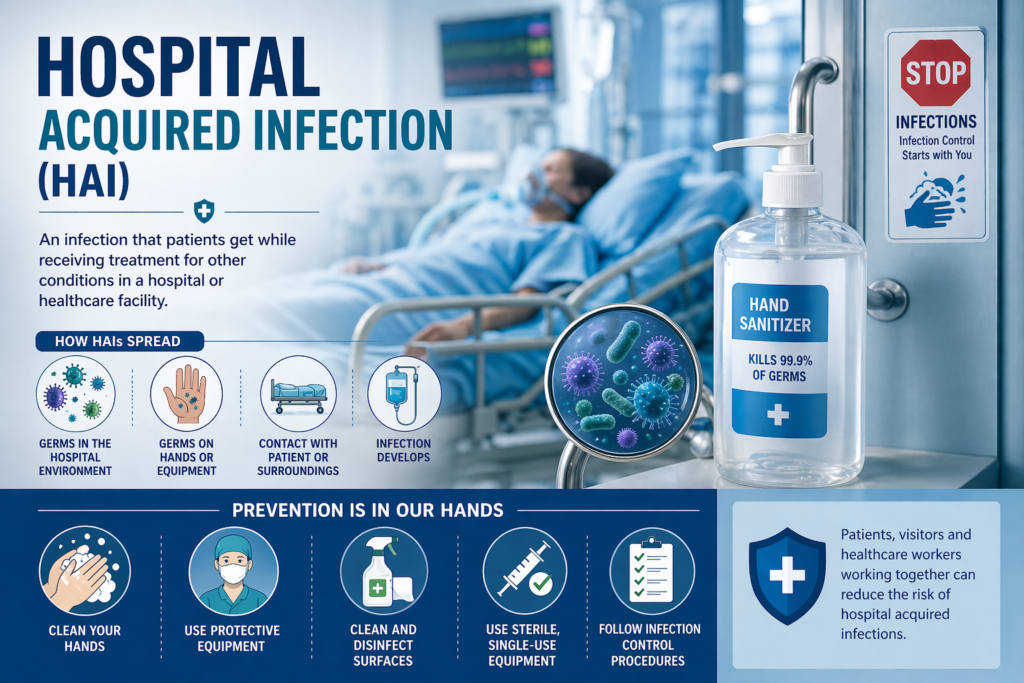
Hospital acquired infections are infections that patients develop at least 48 hours after admission to a healthcare facility. These infections were not present or incubating at the time of admission. They can occur in hospitals, nursing homes, rehabilitation centers, outpatient clinics, and other healthcare settings.
The shocking truth is that hospital acquired infections affect approximately 1 in 31 hospitalized patients on any given day. This translates to hundreds of thousands of infections annually, making it a critical public health issue that demands immediate attention.
These infections develop because healthcare environments bring together vulnerable patients with weakened immune systems, invasive medical procedures, and potential exposure to antibiotic-resistant bacteria. The combination creates a perfect storm for infection transmission.
The 5 Most Common Types of Hospital Acquired Infections
1. Catheter-Associated Urinary Tract Infections (CAUTI)
Urinary tract infections linked to catheter use represent the most frequent type of hospital acquired infections. When urinary catheters remain in place for extended periods, bacteria can travel up the catheter into the bladder, causing painful and potentially dangerous infections.
These infections account for approximately 32% of all healthcare-associated infections reported by acute care hospitals. The longer a catheter stays in place, the higher the infection risk becomes.
2. Surgical Site Infections (SSI)
Surgical site infections occur at the incision area after surgery. Despite strict sterile protocols, bacteria can enter the surgical wound during or after the procedure. These infections can be superficial, involving only the skin, or deep, affecting tissues beneath the skin and organs.
Surgical site infections complicate recovery, extend hospital stays, and significantly increase healthcare costs. They represent about 22% of all hospital acquired infections.
3. Central Line-Associated Bloodstream Infections (CLABSI)
Central lines are catheters placed in large veins to deliver medications, fluids, or nutrition. When bacteria enter the bloodstream through these lines, serious infections can develop. Central line-associated bloodstream infections carry a mortality rate of 12-25%, making them particularly deadly.
4. Ventilator-Associated Pneumonia (VAP)
Patients on mechanical ventilators face elevated risks of developing pneumonia. The breathing tube can allow bacteria to enter the lungs, causing severe respiratory infections. Ventilator-associated pneumonia typically develops 48 hours or more after intubation.
This type of infection is especially concerning because it affects already critically ill patients whose immune systems are compromised.
5. Clostridioides difficile (C. diff) Infections
- difficile causes severe diarrhea and intestinal inflammation. This bacterium spreads easily in healthcare settings, particularly after antibiotic use disrupts the normal gut bacteria. C. diff infections are notoriously difficult to treat and can recur multiple times.
Major Causes Behind Hospital Acquired Infections
Understanding the root causes helps in prevention. Hospital acquired infections develop through several pathways:
Invasive Medical Devices: Catheters, ventilators, and IV lines create direct pathways for bacteria to enter the body. Each device insertion point represents a potential entry site for harmful microorganisms.
Antibiotic Overuse: Excessive antibiotic use creates resistant bacteria strains that are harder to eliminate. These superbugs thrive in hospital environments where antibiotics are commonly used.
Contaminated Surfaces: Hospital rooms, medical equipment, and frequently touched surfaces can harbor dangerous pathogens. Despite rigorous cleaning protocols, bacteria can survive on surfaces for extended periods.
Healthcare Worker Transmission: When medical staff fail to follow proper hand hygiene protocols, they can inadvertently transfer bacteria from one patient to another. Studies show that hand hygiene compliance rates often fall below 50% in busy hospital units.
Overcrowding: Crowded facilities with insufficient space between patients facilitate infection spread through airborne particles and contact transmission.
Compromised Immune Systems: Hospitalized patients often have weakened immune defenses due to underlying illnesses, surgeries, or medications, making them more susceptible to infections.
Warning Signs and Symptoms You Shouldn't Ignore
Recognizing hospital acquired infections early improves treatment outcomes. Watch for these critical warning signs:
- Fever developing 48 hours or more after hospital admission
- Redness, swelling, or discharge at surgical sites or catheter insertion points
- Increased pain or tenderness around wounds
- Difficulty breathing or chest pain
- Sudden changes in mental status or confusion
- Persistent diarrhea, especially after antibiotic treatment
- Unusual fatigue or weakness
If you or a loved one experiences any of these symptoms during or shortly after hospitalization, immediately notify healthcare providers.
Powerful Prevention Strategies That Actually Work
Prevention remains the most effective weapon against hospital acquired infections. Both healthcare facilities and patients play crucial roles.
For Healthcare Facilities:
Strict Hand Hygiene Protocols: Healthcare workers must wash hands before and after every patient contact. Studies from the World Health Organization demonstrate that proper hand hygiene can reduce infection rates by up to 50%.
Device Minimization: Removing unnecessary catheters, IV lines, and other devices as soon as medically appropriate drastically reduces infection risks.
Environmental Cleaning: Regular, thorough disinfection of patient rooms, medical equipment, and high-touch surfaces prevents pathogen transmission.
Antibiotic Stewardship: Prescribing antibiotics only when necessary and choosing the appropriate type and duration helps combat antibiotic resistance.
Isolation Protocols: Separating patients with contagious infections prevents disease spread to vulnerable individuals.
Staff Education: Continuous training ensures healthcare workers stay updated on best infection prevention practices.
For Patients and Families:
Ask Questions: Don’t hesitate to ask doctors and nurses whether catheters or other devices are still necessary. Patient advocacy saves lives.
Hand Hygiene Reminders: Politely remind healthcare workers to wash their hands before touching you. Most professionals appreciate this reminder.
Visitor Restrictions: Limit visitors, especially those who are sick. Each additional person in the room increases infection exposure risks.
Personal Hygiene: Maintain your own hand hygiene and encourage family members to do the same.
Speak Up: Report any concerns about cleanliness or symptoms immediately. Early detection enables prompt treatment.
The Devastating Impact on Healthcare Systems
Hospital acquired infections impose tremendous burdens on healthcare systems worldwide. According to the Centers for Disease Control and Prevention, these infections result in:
- Approximately 99,000 deaths annually in the United States alone
- Extended hospital stays averaging 7-10 additional days per infected patient
- Healthcare costs exceeding $28-45 billion per year
- Emotional trauma for patients and families
- Legal liabilities for healthcare institutions
These staggering numbers highlight why hospital acquired infections represent a critical priority for healthcare quality improvement initiatives.
Emerging Technologies Fighting Hospital Acquired Infections
Innovation offers hope in the battle against these infections. New technologies include:
Antimicrobial Surfaces: Copper-infused materials and self-disinfecting surfaces kill bacteria on contact, reducing environmental contamination.
UV Disinfection Robots: Automated robots use ultraviolet light to sterilize patient rooms between occupants, eliminating pathogens that traditional cleaning might miss.
Electronic Monitoring Systems: Digital systems track hand hygiene compliance, alerting staff when they forget to sanitize.
Rapid Diagnostic Tests: New testing methods identify infections and resistance patterns within hours instead of days, enabling targeted treatment.
Probiotic Therapies: Beneficial bacteria supplements may help prevent C. difficile infections by maintaining healthy gut microbiomes.
The Role of Antibiotic Resistance in Hospital Acquired Infections
Antibiotic resistance makes hospital acquired infections increasingly dangerous. Bacteria evolve to survive common antibiotics, creating “superbugs” like MRSA (methicillin-resistant Staphylococcus aureus) and VRE (vancomycin-resistant enterococci).
These resistant organisms spread rapidly in healthcare settings because:
- Antibiotics kill susceptible bacteria, allowing resistant strains to multiply
- Close patient proximity facilitates transmission
- Invasive procedures provide entry points for resistant bacteria
The National Institutes of Health emphasizes that combating antibiotic resistance requires coordinated efforts including judicious antibiotic use, infection prevention, and new drug development.
Your Rights as a Patient
Patients have fundamental rights regarding infection prevention:
- Right to Information: You can ask about the hospital’s infection rates and prevention measures
- Right to Cleanliness: Expect clean rooms, equipment, and environments
- Right to Question: Challenge any procedure or practice that seems unhygienic
- Right to Refuse: Decline unnecessary invasive devices or procedures
- Right to Advocacy: Have family members or advocates present to help ensure proper care
Exercising these rights empowers patients to participate actively in their safety.
Recovery and Long-Term Consequences
Hospital acquired infections can have lasting effects beyond the initial illness. Some patients experience:
- Prolonged recovery periods requiring extensive rehabilitation
- Chronic pain or disability from severe infections
- Psychological trauma including anxiety about future healthcare encounters
- Financial hardships from extended treatment and lost work time
- Reduced quality of life
Comprehensive follow-up care and support systems are essential for patients recovering from serious hospital acquired infections.
The Future of Infection Prevention
Healthcare systems worldwide are implementing comprehensive strategies to eliminate hospital acquired infections. These initiatives include:
- National surveillance systems tracking infection rates
- Public reporting of hospital infection statistics
- Financial penalties for facilities with high infection rates
- Mandatory infection prevention training for all healthcare workers
- Patient education programs starting before hospital admission
According to research published in Medscape, hospitals implementing bundled prevention strategies have achieved remarkable infection rate reductions of 50-70%.
Take Action Today
Hospital acquired infections represent preventable tragedies. Whether you’re a patient, family member, or healthcare worker, you hold power to make a difference.
Before your next hospital visit, educate yourself about infection risks. During hospitalization, stay vigilant about hand hygiene, ask questions, and speak up about concerns. After discharge, monitor for infection symptoms and seek immediate medical attention if they appear.
Remember, hospital acquired infections affect millions, but together we can dramatically reduce these numbers. Your awareness and advocacy can save lives—starting with your own.
Conclusion
Hospital acquired infections remain a critical healthcare challenge affecting patients worldwide. By understanding the types, causes, and prevention strategies, we can collectively work toward safer healthcare environments. Whether you’re preparing for a hospital stay or supporting a loved one, knowledge empowers protection. Stay informed, stay vigilant, and don’t hesitate to advocate for proper infection control measures. Your health and safety depend on it.
Frequently Asked Questions (FAQ)
What is a hospital acquired infection (HAI)?
A hospital acquired infection (HAI) is an infection that a patient develops during their stay in a hospital or healthcare facility, which was not present at the time of admission.
What are common types of hospital acquired infections?
Common HAIs include:
- Urinary tract infections (UTI)
- Surgical site infections (SSI)
- Bloodstream infections
- Pneumonia (especially ventilator-associated)
What causes hospital acquired infections?
HAIs are caused by bacteria, viruses, or fungi. Common causes include poor hygiene, contaminated equipment, invasive procedures, and weakened immunity.